CHOOSE GATEWAY
Your pet is special.
They deserve a specialist.
FOR PET OWNERS
Your pet having surgery can be a stressful time.
Gateway Veterinary Surgery (GVS) was founded to make that experience easier on your entire family. GVS partners with your regular veterinarian to bring you a boarded veterinary surgical specialist working with the vet you have chosen for the care of your pets for years. This team approach allows the balance of convenience while still offering the expertise of a surgical specialist in your family’s regular vet office.
FOR VETERINARIANS
GVS is Here to Help You and Your Patients.
SERVICES
What We Offer
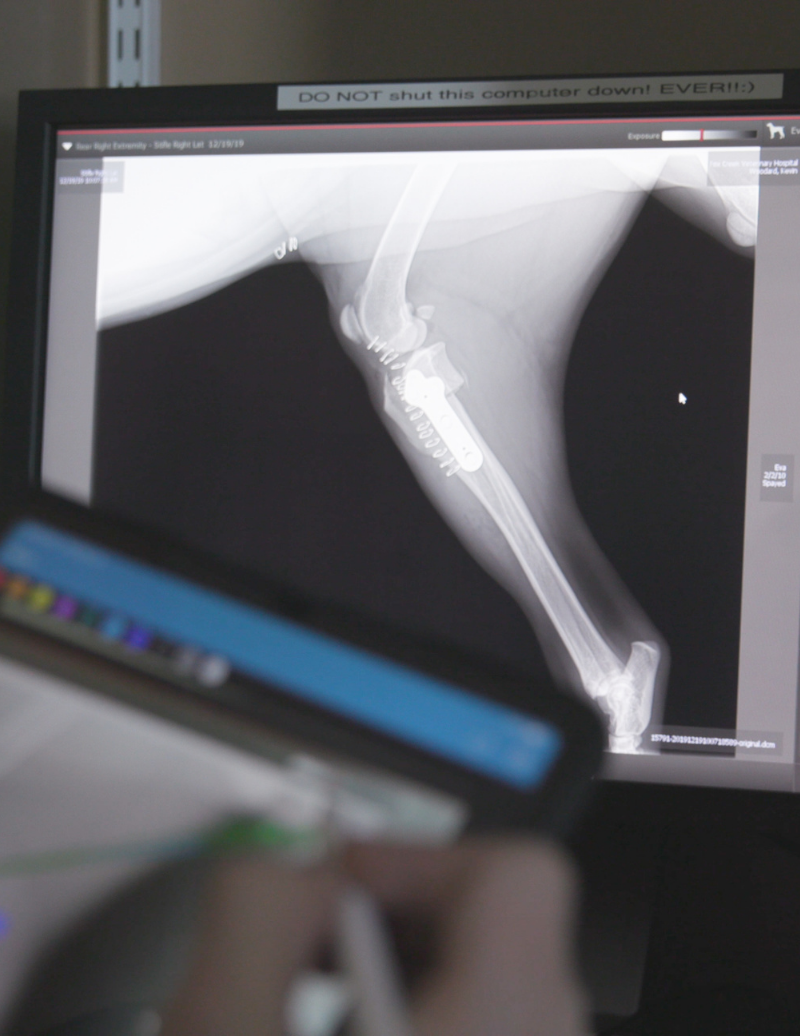
Pet TPLO
TPLO surgery is performed on dogs with the aim of stabilizing the animal’s knee after they tear the cranial cruciate ligament.

Pet Orthopedic
We provide the best-in-class surgery for any and all orthopedic-related injuries. Our veterinary services aim for a speedy recovery.

Pet Soft Tissue/ Oncologic

Pet Consultations
Designed to help pet owners explore the various options and proceed to make the best decision for you and your pet.
TPLO
HAPPY CLIENTS
Thank you for making us one of the highest-rated veterinary specialists in St. Louis, MO!
Your feedback means so much to us. Thank you for allowing us to care for your pets.